Treatments
- Rehabilitation For Impaired Vision
- Photodynamic Treatment
- Gas Tamponade
- Glaucoma Treatmens
- Injections Of Medication Into Eye
- Eyelid Surgery
- Obstruction Of The Tear Ducts
- Cataract Treatment
- Laser Trabeculoplasty
- Premature Retinopathy (ROP)
- Pterygium Surgery
- Refractive Laser Surgery
- Retina Diseases and Treatment
- Silicone Oil Tamponade
- Strabismus Surgery
- Vitrectomy Surgery
Glaucoma Treatmens
Disruption to the internal eye fluid or increased resistance to the external flow results in internal pressure more than the eye can tolerate and thereby a group of diseases characterised by irreversible damage to the optic nerve.
In open nagle tyoe glaucoma, the disease gives no indications until the advanced stage at which vision loss develops. The progressive course of the disease is generally slow and initially the patient is not aware of impairments in the field of vision.
Figure 1. Filtering bleb of trabeculectomy 12 months after surgery.

In acute closed angle type glaucoma the prevention of internal eye fluid circulation results in high levels of internal eye pressure. In these cases, clouded vision, coloured circles around light, severe pain in and around the eye, redness of the eye and nausea and vomiting may be seen. In congenital glaucoma cases, there are findings of watering of the eyes, large diameter cornea and loss of clarity.
The risk factors in primary open angle glaucoma are advanced age, negro ethnicity, positive family history, diabetes, low blood pressure and myopia.
The risk factors in primary closed angle glaucoma are advanced age, Caucasian ethnicity, positive family history and female gender.
In addition glaucoma may develop associated with eye trauma, infection inside the eye, steroid use, contact lenses, neovascularisation of the iris and structural changes of the anterior segment of the eye.
Following biomicroscopy measurement of internal eye pressure, optic disc and gonioscopic angle examination, diagnosis is made by the visual field test and analysis of the optic nerve fibres by tomography.
It is also surgery applied to patients whose intraocular pressure cannot be reduced to the desired level, in order to allow the intraocular fluid to be extracted from the eye in an effective way, thus reducing this pressure.
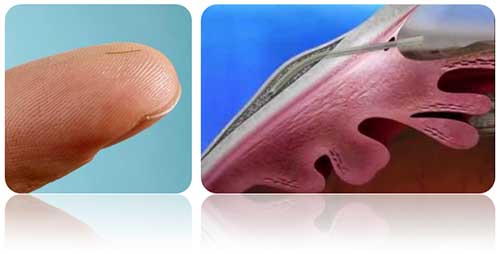
Figure 2. External (left) and intraocular (right) appearance of minimally invasive glaucoma surgery implant.
Another known method is trabeculectomy. In this method, the operation is made on the sclero-corneal intersection point where the white part of the eye and trabeculum are located. The intraocular fluid passes through the created fistula and is collected in the created reservoir. The purpose of this method is to have the intraocular fluid reach the reservoir sac, gather here, and mix with the bloodstream. Antibiotic treatment should continue after surgery to prevent infection.
Some special medications should be used during the operation in order to prevent the obstruction of the newly created reservoir due to scar formation and an increase in the connective tissues developing because of wound healing in the surgical area. In spite of all precautions, obstructions in the reservoir may occcur after a while and there may be a need to use medications again to reduce intraocular pressure.




